Predictive Analytics in Healthcare: Unlocking Insights

Table of Contents
Predictive analytics in healthcare increasingly forecasts operational and revenue shortages in addition to disease and early care. In the healthcare industry, specialists evaluate vast amounts of patient data to forecast illnesses, but occasionally, a tiny quantity of missing data might make it challenging to do so. Patients only visit hospitals when they start experiencing symptoms. Certain diseases become serious with time and make it challenging for medical professionals to manage their patients' health.
Predictive analytics can help predict certain symptoms before they occur. It helps in the early treatment of the patient and generates insights that allow accurate decision-making. This reduces misleading assumptions and enhances personalized care. There are several predictive analytics accessible for different applications. This optimizes workflow and improves operational efficiency.
What is Predictive Analytics in Healthcare, and Why Does It Matter
In order to forecast operational and health issues, predictive analytics in healthcare integrates data with artificial intelligence and machine learning technologies. This helps to reduce risk, make better decisions, and implement measures to reduce operating gaps.
The following are some of the reasons that predictive analytics is most important:
- Enables early diagnosis and prevention.
- Reduces hospitalizations and problems.
- Proactive treatment enhances patient outcomes.
- Optimizes personnel, bed capacity, and resource use.
- Reduces expenses and operational inefficiencies.
- Improves data-driven clinical decision-making.
How Predictive Analytics in Healthcare Works
Collect large datasets
Predictive analytics in healthcare begins with the collection of huge quantities of clinical data from electronic health records, diagnostics, imaging, pharmaceutical data, wearable vitals, and patient history. This data in one location is critical for accurate risk prediction and population health insights.
Clean and organize the data
Raw medical data is messy. Healthcare data analytics eliminates errors and closes gaps for advanced data processing and connectivity frameworks. In order to improve the performance of machine learning algorithms, this ensures that each data point is accurate and consistent.
Identify patterns using machine learning
Millions of data points are then analyzed by machine learning algorithms to identify operational inefficiencies, disease development patterns, and early danger indications. Predictive analytics in the healthcare industry can use this pattern recognition to find signs that doctors might not be able to identify for prediction.
Generate predictions about future risks
Machine learning algorithms analyze Millions of data points to identify operational inefficiencies, disease development patterns, and early danger indications. Predictive analytics in the healthcare industry can use this pattern recognition to find signs that doctors might not be able to identify for prediction.
Provide actionable insights to clinicians
In the end, the insights show up in current workflows via dashboards, decision-support tools, and alerts. Predictive analytics in healthcare provides practical suggestions that enhance patient safety, reduce workload, and facilitate quicker decision-making.

Key Applications of Predictive Analytics in Healthcare
Disease risk prediction
Machine learning models predict early risk for diabetes, cancer, and heart disease using lab results, vital signs, lifestyle data, and medical history. This enables medical practitioners to respond before the condition gets worse.
Hospital readmission prediction
Predictive insights determine which patients are most likely to come back within some days for care. This enables teams to close follow-up gaps and improve discharge plans.
Sepsis early detection
Clinicians have an earlier window to respond to early treatment because real-time analytics detects minor warning indicators.
Patient deterioration monitoring
For teams to react effectively before a crisis arises, continuous monitoring helps identify early signs of worsening.
Operational predictions
Hospitals can stay organized, cut down on delays, and effectively manage resources by using forecasts for staffing, bed occupancy, and ED surges.
Chronic disease management
Long-term data patterns show when individuals with chronic conditions require care. This promotes preventive and individualized care.
Fraud detection in claims
Predictive analytics in healthcare reduces fraud and protects healthcare resources through the detection of irregular billing patterns.
Benefits of Predictive Analytics in Healthcare
Faster diagnosis and early intervention
By identifying minor risk patterns long before they show up in assessments, predictive analytics in healthcare speeds up decision-making. This enables medical professionals to take action when a disease is in its early and treatable stages.
For instance, a sepsis prediction model alerts medical staff approximately four to six hours before the onset of symptoms. This makes it possible to provide antibiotics immediately and stops ICU escalation.
Personalized patient treatment
Health data analysis provides strategies for optimized treatment. It is based on lifestyle information, response to medication, trends in disease progression, and individual risk profile.
For instance, when analyses indicate increased fluid retention, a patient with heart failure receives an adapted medication change.
Reduced costs and fewer errors
Predictive analytics in healthcare promotes cost-effective treatment and reduces preventable medical errors. To this end, it identifies high-risk patients early and cuts down on redundant testing, thereby providing financial stability and security.
For instance, the prediction of the patient's readmission risk allows for rapid follow-up coordination. This prevents expensive hospitalization expenses, and administrative errors are also reduced.
Better resource planning
Hospitals can predict patient load, bed occupancy, staffing shortages, and ED growth through healthcare services. This guarantees that teams use resources efficiently.
For instance, a hospital actively recruits emergency personnel when analyses indicate a 22% increase in admissions over the weekend. Therefore, patients have shorter waiting times and fewer disturbances.
Improved clinical outcomes
Predictive insights provide continuous information that enables fewer avoidable problems, accurate monitoring, and early intervention. This gives better results for the patients.
For instance, by continuously monitoring a patient's breathing, predictive analytics in healthcare can alert specialists hours before a patient's condition worsens. It provides rapid oxygen support and helps prevent serious breathing problems.
Challenges of Predictive Analytics in Healthcare
Poor or incomplete data
When clinical data is absent, inaccurate, or separated across systems, predictive analytics in the healthcare industry struggles, which immediately lowers the accuracy of risk forecasts.
Early-warning models are weakened by incomplete histories or missing vital signs.
How to deal with it:
To ensure complete datasets, employ automated data validation, enforce documentation quality, and build more robust data pipelines.
Integration with legacy systems
Healthcare data analytics often face difficulties as a result of outdated EHRs, disconnected systems, and incompatible formats, which slow down the use of data analytics.
EHR, billing, and laboratory systems that are not connected prevent the creation of integrated patient insights.
How to deal with it:
To smoothly integrate current systems with the new platform, use contemporary APIs, sequential integration layers, and interoperability standards like HL7 or FHIR.
Model bias and fairness issues
Bias from past data may be inherited by machine learning models, which could reduce accuracy for specific patient groups and raise issues with fairness.
Risk scores for underrepresented populations are less accurate.
How to deal with it:
To guarantee equitable predictive performance, use a variety of training datasets, conduct fairness audits, and implement mitigation of bias strategies.
Clinician trust and adoption
Without clinical support, even accurate models fall short. For forecasts, clinicians require clear and understandable insights.
When a model explains why a risk alert was created, providers trust it.
How to deal with it:
Make use of explainable AI that gives concise explanations for forecasts, and naturally incorporate findings into current healthcare processes.
Regulatory compliance
Deployment of healthcare data analytics is difficult and time-consuming due to strict privacy, security, and transparency regulations.
Audits and approvals may cause a delay in implementation.
How to get past it:
Use compliant data handling procedures, establish robust governance, keep detailed audit logs, and connect with compliance teams for the start of the project.
Use Cases of Predictive Analytics in Healthcare
Forecast for patient absences
To estimate whether patients are likely to miss appointments, algorithms consider their historical behavior, appointment scheduling, and demographics. This decreases the time gap, which helps hospitals to actively re-engage patients.
Early indicators of health hazards
Health data analysis can identify high-risk signals and behavioral changes. Doctors receive notifications and are allowed to intervene before the problem worsens.
Recognize high-risk pregnancies
Predictive analytics in healthcare uses vital signs, medical history, and laboratory patterns to detect issues early. This promotes safe pregnancy care and careful observation.
Forecasting medication compliance
Models anticipate which patients will discontinue their medications based on behavioral and clinical trends. Care teams can make timely reminders or changes.
ER demand forecasts
Analytics predicts community-level triggers, seasonal fluctuations, and peak hours. This helps hospitals to adjust staffing and bed arrangements to prevent overcrowding.
Identifying stroke-risk patients
Analytics identify persons at risk of stroke by analyzing vital signs, lifestyle information, and previous incidents. With this, specialists provide preventive and proactive care.
Making surgical scheduling efficient
Predictive models estimate case durations, cancellation rates, and resource requirements. This improves patient flow, reduces delays, and boosts OR utilization.
Framework and Technologies for Predictive Analytics in Healthcare
| Category | Components and Tools | Explaination |
| Data Sources | DNA/Genomics, EHRs, Claims, and Medical Imaging | Predictive analytics in healthcare depends on these data sources, which provide a deeper understanding of patient history, current vital signs, genetic risks, and imaging patterns for precise projections. |
| Data Engineering | Data Warehouses and ETL Pipelines | Solid data engineering reduces fragmentation and increases model reliability. This ensures that healthcare data is clean, cohesive, and ready for analysis. |
| Analytics & ML Models | Neural networks, decision trees, and regression | Using large-scale clinical information and pattern recognition, advanced machine learning algorithms assist healthcare professionals in identifying anomalies, predicting illness risk, and customizing care. |
| Cloud Platforms | Snowflake Healthcare Data Cloud, Azure Health Insights, Google Cloud Healthcare API, and AWS HealthLake | These platforms provide scalable, compliant environments designed for safe PHI management, quick model deployment, and health data integration. |
| Visualization Tools | Tableau and Power BI | Clinicians may quickly make data-driven decisions with the help of user-friendly dashboards that translate complex forecasts into actionable ones. |
| MLOps Tools | Kubeflow, Databricks, MLflow, and MLOps | Automation guarantees smooth implementation in actual clinical settings, quicker iteration, and ongoing model monitoring. |
Types of Predictive Analytics in Healthcare
Classification models-
Predictive analytics is used in healthcare to categorize patients into risk groups, such as disease vs no disease, high risk versus low risk, or stable versus worsening. The important uses are early disease diagnosis, sepsis alerts, population risk assessments, and clinical decision support.
Regression models -
Regression algorithms predict length of hospital stay, pharmaceutical dosage requirements, medical response rate, and treatment costs. Regression models are used in analytics to predict trends in demand and patient utilization. Also, helps in maximizing resources, minimizing operational inefficiencies, and making value-based care decisions.
Clustering models-
Clustering discovers distinct patient segments using symptoms, behaviors, or past data. Socioeconomic characteristics are helps for group identification, individualized therapy, chronic illness management, and health analysis. Clustering with AI in health analytics uncovers hidden patterns. This helps to create precise and targeted treatment plans.
Time-series forecasting-
Time series forecasting models predict future admissions, emergency department demand, intensive care unit occupancy, seasonal disease outbreaks, or supply chain demands. These models help hospitals to optimize workforce optimization, capacity planning, and improve operational efficiency.
Survival analysis -
Survival analytics predicts the probability and timing of clinical outcomes. This includes readmission, relapse, treatment failure, and patient death. It provides information for proactive care management, chronic illness monitoring, and risk assessment. Hospitals use Survival analysis to patient with risk for patients and provide them personalized care.
Comparison of Predictive Analytics in Healthcare with Other Healthcare Analytics
| Type of Analytics | Question It Answers | Description | Example in Healthcare |
| Descriptive Analytics | What happened? | Recaps past medical data to highlight trends and patterns. This helps hospitals in comprehending patient behavior and historical performance. | Monthly reports on patient admissions. |
| Diagnostic Analytics | Why did it happen? | Employs deeper analysis to determine the underlying reasons for clinical or operational incidents. | Looking for the reason behind an epidemic of a disease. |
| Predictive Analytics | What will happen? | Forecasts future dangers, clinical events, or operational demands in the healthcare industry using machine learning and predictive analytics. | Anticipating high-risk cardiac arrest several hours in advance. |
| Prescriptive Analytics | What should we do? | Combines prediction and decision models to suggest the best course of action for administrators and clinicians. | Recommending a patient's optimal course of treatment. |
Metrics to Evaluate Predictive Models in Healthcare
Precision
It determines how often the model's predictions are accurate across the entire data set. It includes positive and negative predictions.
High accuracy ensures that your predictive model serves large health data sets consistently and flawlessly.
The sepsis prediction model accurately diagnosed patients in 93 out of 100 cases.
Efficiency
It shows the percentage of high-risk patients who are at high risk. It focuses on the accuracy of optimistic forecasts.
This helps to reduce false positives, unnecessary alerts, and the burden of non-critical patients on the part of doctors.
The heart failure risk model ensures that the majority of alarm cases actually require immediate intervention, even if a small number of patients are identified.
Sensitivity
This assesses the model's ability to identify risky patients. Missing high-risk patients can lead to negative results and delayed diagnosis. This provides better security results.
95% of high-risk patients can be identified by stroke prediction systems before symptoms appear.
Specification
This assesses how well the model detects patients who are not in the risk zone.
High specificity reduces alert fatigue, prevents false alarms, and maintains physician confidence in AI.
A decomposing model prevents stable patients from being falsely classified as critical.
AUC-ROC (Area Under the Receiver Operating Characteristic Curve)
This summarizes the model's ability to distinguish between patients who are in the risk zone and those who are not. It considers all the criteria.
Provides a metric to evaluate model reliability across a variety of challenging scenarios and demographics.
A model with an AUC of 0.92 consistently distinguishes patients whose condition worsens from those who are stable in hospital units.
Explainability Tools for Healthcare Predictive Models
| Tool / Detailed Explanation | How It Supports Clinicians and Healthcare Workflows | Example in Healthcare |
| SHAP (SHapley Additive Explanations)It demonstrates how each feature, such as labs, vitals, demographics, and medical history, influences the final forecast using concepts from game theory. | This increases confidence, fosters openness, and helps medical professionals understand why a model identified a patient as high-risk. This is essential for ethical AI and regulatory compliance. | A SHAP graph demonstrating that the most common reasons a deterioration model identified a patient were increased respiratory rate and decreasing SpO₂. |
| LIME (Local Interpretable Model-Agnostic Explanations)This provides predictions that help patients comprehend complicated models. | This helps clinicians justify judgments in charts, interdisciplinary meetings, or audits and validate forecasts on an individual basis. | As per the LIME method, an individual's recent ER visits and medication gaps were the primary causes of their elevated readmission risk. |
Workflow of Predictive Analytics in Healthcare
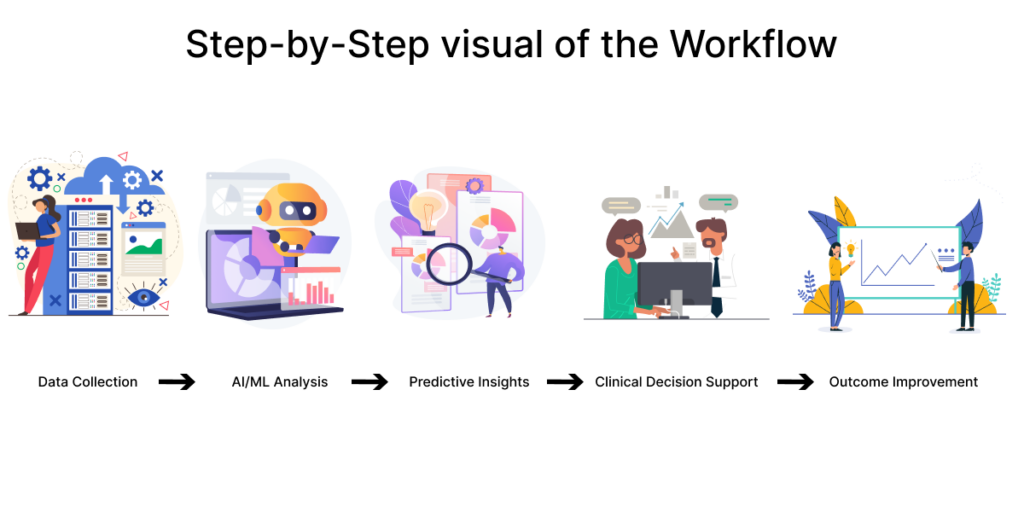
Data Collection
- Start collecting a variety of information from patient history, radiology scans, lab results, and EHR records. Accurate predictive analytics in healthcare is supported by this foundation.
AI/ML Analysis
- Data is cleaned, standardized, and integrated into the system to remove errors, fill gaps, and provide an accurate source. For better analysis of healthcare services, this is important.
- Experts convert raw data into valuable clinical signals. This includes trends in vital signs and disease patterns. Because of this, machine learning models become more applicable in clinical settings.
Predictive Insights
- Patient data from the past is used to train machine learning and deep learning models. This makes it easier to spot trends that point to danger, deterioration, and expected results.
- To ensure that the models perform consistently, they are tested using health metrics, including precision, recall, and AUC.
Clinical Decision Support
- After validation, the predictive model is integrated into hospital workflows, including dashboards, alarms, and EHR systems. This facilitates the delivery of clinical decision support in real time.
Outcome Improvement
The performance of the model is regularly tested. This helps detect data drift, maintain accuracy, and retrain the system in response to changing health trends.
Best Practices for Implementing Predictive Analytics in Healthcare
Start with a small pilot
Predictive analytics in healthcare starts with a measurable use case. This could be predicting sepsis, reducing readmission rates, or predicting the need for an emergency department. Hospitals can start small by getting clinical feedback, showing a quick return on investment, and building momentum for using AI.
Build a cross-functional team
To achieve high-performance analytics for healthcare, physicians, data scientists, IT teams, compliance officers, and operations managers work together. This guarantees that the model is suitable for medical treatment.
Ensure data quality before modeling
Reliable predictive modeling is built on clean, consistent, and integrated data. Model accuracy and clinical reliability are improved by improving EHR consistency, reducing missing values , and facilitating system interoperability. These help form the building blocks for better health data analysis.
Use explainable AI for clinical trust
Clinicians can better comprehend why a patient was identified as high risk by using explainability tools such as SHAP and LIME. Gaining trust and guaranteeing the responsible application of AI in medical contexts depend on this transparency.
Integrate predictions into daily workflow
Predictive analytics must be integrated into current EHR dashboards, clinical decision support systems, or bedside monitoring technologies to have a significant impact. With this forecasting, Specialists can take fast actions.
Train medical staff to interpret AI outputs
Medical experts require precise instructions on how to comprehend model explanations, read risk scores, and follow suggested courses of action. Adoption is strengthened by hands-on training sessions, so predictive models improve clinical judgment.
Maintain compliance and data governance
Strict guidelines for security, fairness, and privacy must be followed while using predictive analytics in healthcare. Throughout the care continuum, safe, moral, and legally compliant AI is ensured by frequent model audits, regulatory governance, bias monitoring, and open documentation.

Future Trends in Predictive Analytics Healthcare
EHR alerts in real-time
EHRs will quickly display predictive information, enabling physicians to respond to danger immediately as it materializes.
Customized healthcare using genomics
Personalized medicine and treatment programs will be possible by genetic information and biomarkers.
Digital twins of patients
Clinicians will be able to simulate therapy outcomes before implementing them in real life with virtual patient replicas.
Predictive models combined with generative AI
AI will mimic clinical situations, enhancing judgment and readiness for challenging situations.
Federation of learning
By working together to train models without exchanging raw data, hospitals will improve compliance and privacy.
AI-powered surveillance robots
Compared to traditional monitoring, robots will continuously monitor patients and anticipate deterioration.
Systems for predictive public health
Accurate forecasting of outbreaks, demand spikes, and community health threats will happen through real-time analytics.
Conclusion
Predictive analytics helps healthcare businesses identify danger earlier, respond faster, and deliver accurate and individualized treatment by combining clinical, operational, and financial data into useful insights.
It is true worth that is seen in increasing operational effectiveness, financial performance, and organizational flexibility, in addition to clinical outcomes. Predictive analytics has measurable effects on the healthcare system, from cutting down on diagnostic delays and readmissions to maximizing personnel, capacity, and compliance.
Accurate and accessible models, interoperable technologies, and high-quality data are essential for successful predictive analytics implementation. This strengthens governance and fosters practitioner trust. Healthcare executives will gain long-term clinical and competitive advantages if they go beyond pilots and integrate predictive intelligence into routine procedures.
To overcome technical obstacles, rely on the best software providers who offer superior solutions. Patoliya Infotech offers the best technological solutions that are secure and reliable.