How to Modernize Legacy System in Healthcare

Table of Contents
Legacy system in healthcare pose the greatest threat to hospitals and management. Imagine you're transferring money with your ancient cell phone. Suddenly, it turns off or hangs, and you become concerned about the security of your account. Just like this, a single error in EHR can cause hospitals to lose all of their data. One single error during an emergency can lead to a dangerous condition for the patient. Legacy systems include EHRs, HIS, LIS, billing platforms, PACS, and a wide range of clinical and administrative applications.
Many systems may not even comply with rules or poor quality due to their age. The outdated system delays operations and makes it difficult to interface with newer technology. A high-quality, compliance-friendly system is important since it is worthwhile in the long run.
What Counts as a Legacy System in Healthcare?
- Outdated EHR/EMR systems that are unable to adapt to contemporary workflows.
- On-premises systems that restrict scalability, like HIS, LIS, and RIS.
- Outdated billing and RCM software that is draining Time and accuracy.
- Paper-based procedures and fragmented applications that disturb continuity.
- Systems lacking interoperability or mobile access.
And there is actual pain of,
- Poor performance and mounting technical debt.
- Growing maintenance costs and vendor lock-in.
- Inability to integrate with APIs, PACS, HL7, and FHIR.
- Data silos that undermine decision-making and analytics.
A Comprehensive Modernization Roadmap For Legacy System in Healthcare
Business Case and System Audit
- Determine what blocks interoperability, slowing down care, or raising technological debt first.
- This includes paper-based workflows, disconnected billing systems, on-premises HIS, and outdated EMRs.
- It requires measuring integration gaps, claim errors, workflow delays, and downtime of the legacy system in healthcare.
- For instance, a multispecialty hospital finds that new FHIR-based apps cannot be integrated with its 14-year-old EMR, which results in a 22% delay in patient registration.
Strategy for Data Migration and Cleaning
- Data must be cleaned, standardized, and mapped into modern formats like FHIR, HL7, ICD, CPT, LOINC, etc., before any modernization.
- The main objective is to eliminate duplicates, resolve patient identity problems, and prepare data for cloud environments.
- For instance, to improve clinical accuracy, the IT team uses a Master Patient Index to combine 3,500 duplicate patient records discovered through data profiling.
Select the Right Modernization Strategy
- Based on scalability, security, compliance, and cost, you have to assess build vs buy vs integrate.
- Many systems benefit from the strangler-pattern approach of architecture. This can be wrapping legacy systems with APIs, while others require a complete redesign or replacement.
- For instance, the company adds an API layer to enable secure FHIR endpoints rather than replacing the entire HIS. This allows for quicker integrations without any downtime.
Pilot Stage and Iterative Implementation
- A modernization effort that begins small is more likely to succeed of a legacy system in healthcare.
- In a controlled setting, you start a pilot, test workflows with clinicians, get input, make adjustments, and then grow.
- For instance, after modernization, the radiology department was selected as the pilot, reducing report delivery times from six hours to one hour.
Integration with Back-Office and Clinical Systems
- This is where true change takes place.
- Using APIs, HL7, FHIR, DICOM, and integration engines, you link the new system to lab systems, PACS, pharmacy, billing, scheduling, and patient apps.
- Instead of being a secondary concern, interoperability becomes a fundamental competency.
- For instance, Lab findings now quickly sync with the new EHR. This decreases clinical errors with manual data entry.
Constant Optimization and Monitoring
- Following deployment, adoption, security, performance, and compliance are tracked.
- Dashboards monitor cloud costs, workflow efficiency, clinical turnaround times, and uptime.
- This keeps the system up to date and prevents it from becoming a legacy of the future.
- For instance, the hospital uses analytics to increase appointment throughput by 27% and decrease claim denials by 18% after going online.
Key Technologies That Enable Modernization in Legacy System in Healthcare
Cloud adoption
Hospitals can expand their infrastructure by moving their old systems to cloud settings like hybrid, private, or public. This lessens reliance on outdated on-premise technology and increases uptime. Adopting the cloud is essential to updating any legacy system in healthcare.
Microservices architecture
In the healthcare industry, segmenting a legacy system into microservices allows for independent module deployment, incremental modernization, and quicker feature delivery. Microservices design lowers risk and makes changes to legacy healthcare systems easier.
FHIR/HL7 APIs and platforms for interoperability
Healthcare legacy systems often face interoperability issues. A legacy system may safely communicate data with EHRs, laboratories, imaging, billing, and patient apps by updating with FHIR, HL7, DICOM, and reliable APIs.
Modernization with low or no code
Low-code systems allow for quick digitization of workflows, form automation, and integrations without requiring extensive engineering. This method effectively reduces technical debt while modernizing a legacy system in healthcare.
Modern mobile-first design and UI/UX
In the healthcare industry, updating a legacy system's interface enhances clinician usability, lowers errors, and boosts adoption. When modernizing a legacy healthcare system, a mobile-first and intuitive design is essential for care teams.
Embedded dashboards and analytics
Actionable insights are frequently lacking in healthcare legacy systems. Continuous operational, clinical, and financial indicators are provided by systems with integrated data analysis and dashboards.
Frameworks for healthcare cybersecurity
Modernizing a legacy healthcare system with zero trust, identity access control, encryption, and ongoing threat monitoring improves security architecture.
Modernization Approaches for Healthcare Legacy Systems
| Approach/ Description | When to Use / Pros / Cons | Healthcare Example |
| Re-host (Shift and Lift)Convert the healthcare industry's legacy system from on-premises servers to a public, hybrid, or private cloud architecture without altering the codebase. | When you require quick modernization, cheaper infrastructure, or less downtime.Reduced hosting costs, quick migration, and little disruption.limits performance gains and does not eliminate technical debt. | Moving a 15 year old HIS to AWS to provide reliable hosting and automated backups. |
| Re-platformTo increase performance without sacrificing essential workflows, upgrade the database, operating system, middleware, or runtime. | When rewriting is impractical, yet the system slows down.Enhanced scalability, increased security, and better performance.Requires testing and some code modifications. | Switching to a cloud-managed PostgreSQL database from an antiquated SQL Server EMR. |
| Re-architect (Microservices)For increased versatility, convert monolithic legacy healthcare systems into microservices and modular components. | when you require interoperability, scalability, regular updates, or API capabilities.Easily integrated with FHIR/HL7 systems, highly scalable, and supports DevOps.Longer implementation time and high effort. | Split an outdated RCM suite into separate services for analytics, billing, claims, and payments. |
| Replace and RebuildCreate a completely new system employing contemporary designs like serverless, cloud-native, and low-code platforms. | When integrating the legacy system is unfeasible, outdated, and unsafe.long-term ROI, interoperability, and a future-proof basis.The highest costs are associated with major shifts in the organization. | Rebuilding a longtime LIS with real-time dashboards, mobile access, and a contemporary user interface. |
| Integrate via APIs and Interoperability Layer Utilize middleware, HL7 integration engines, and FHIR APIs to expand the functionality of the legacy system. | When funds are scarce or phased modernization is required.Enhances interoperability, eliminates data silos, and produces quick wins.Legacy restrictions are still in place. | Connecting an outdated EMR to patient interaction and telemedicine applications via an API gateway. |
Governance, Compliance, and Risk Management in the Modernization of a Healthcare Legacy System
Compliance Alignment
Strict adherence to PHI security, access controls, audit logs, retention regulations, and encryption must be ensured by every modernization effort.
- HIPAA-compliant virtual private clouds (VPCs)
- Role-based access (IAM, RBAC)
- Transit encryption and encrypted backups
Risk Evaluation and Analysis of Change Impact
Every workflow improvement needs to be evaluated for operational and clinical risk.
- Will emergency rooms be affected by downtime?
- Will billing accuracy be impacted by data migration?
- Will PACS or LIS connectivity be affected by API upgrades?
Planning for Vendor Transition and Exit
In the healthcare industry, vendor lock-in frequently makes replacing a legacy system challenging.
An appropriate plan must consist of:
- Access to source code
- Handover of documentation
- Audits of licensing
- Timelines for support transitions and clear SLAs
Clinical Safety and Data Validation
Errors in data can have serious medical consequences.
Therefore, modernization needs to incorporate:
- Validation in clinical settings
- reconciliation at the record level
- Accuracy of patient identity (MPI-Master Patient Index)
- Trails of audits
Continuity of Operations and Reduction of Downtime
Hospitals can't afford system outages.
As a result, teams use:
- Blue and green deployments, where blue is the current version and green indicates the modern version
- Phased rollouts
- Strategies for failover
- On-call teams for DevOps
Integration of the Cybersecurity Framework
Legacy system in healthcare make the security posture weaker.
Modernization needs to incorporate:
- Architecture with zero trust
- Threat identification, like SIEM and SOAR
- Governance of identity and access
- Frequent evaluations of vulnerabilities
How to Choose the Right Modernization Approach in a Legacy System in Healthcare
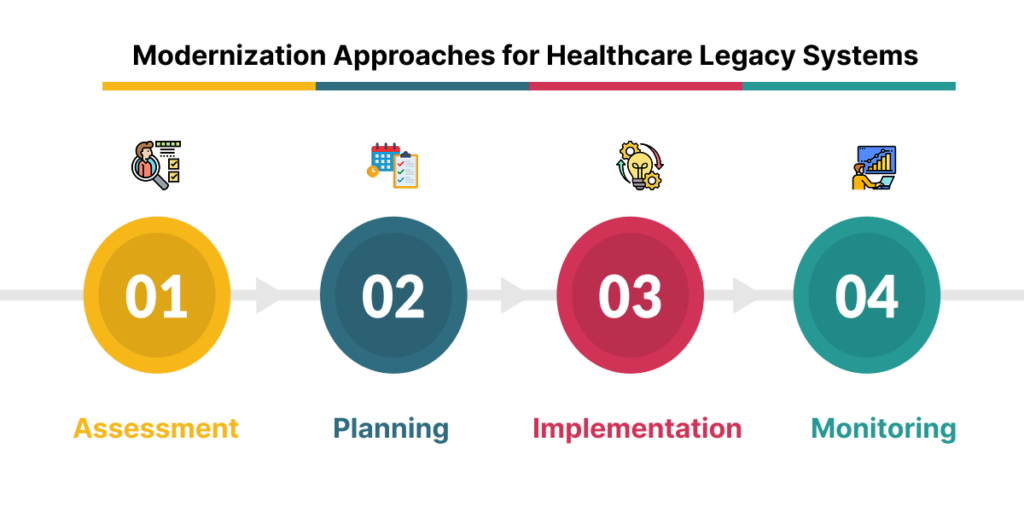
Your current situation and modernization objectives will determine which strategy is best for you.
Select Re-host when:
When a healthcare legacy system is reliable, but on-premise maintenance is costly.
You urgently need improved uptime and less expensive hosting.
You want to begin cloud adoption without massive restructuring.
Re-platform when:
Database constraints and performance bottlenecks have an impact on clinical workflows.
Managing OS upgrades and security patches is challenging on legacy technology.
You want rapid enhancements without a complete rebuild.
Select Microservices for Re-architecting when:
Interoperability with FHIR/HL7 systems is essential.
For patient apps, healthcare workflows, or billing, you demand modular services.
You are shifting toward cloud-native IT solutions for healthcare.
Select Rebuild or Replace when:
The healthcare industry's legacy system is nearing its end of life.
Old architecture is unable to accommodate the additional capabilities that clinical teams require.
A top priority is long-term digital transformation.
Select API Integration When:
You have a tight budget and require quick results.
You want to maintain the basic system while adding FHIR connectivity.
Instead of doing an entire remodel, you intend to modernize in stages.

Conclusion
Healthcare system modernization goes beyond just upgrading IT software. It gives organizations the IT foundational solutions needed for a safe, faster, and value-based approach to Interoperability and the Delivery of Care. Organizations that are successful in their modernization initiatives will benefit from increased efficiencies. This was achieved through improved patient outcomes, lower costs of operation, and greater levels of Compliance.
The first step for achieving these benefits is to take incremental steps, validate progress along the way, utilize intelligent APIs, and continue to scale over time. Organizations need to create a well-defined roadmap with clearly defined stages like data Quality, Cloud Readiness, API Interoperability, Cybersecurity Upgrades, and Clinical Safety Checks. This will have the ability to transition their Legacy systems that do not support these new marketplace requirements into modern, flexible, future-ready platforms.
Companies have to select someone who has proven experience in the development of a new system or in integrating it. This directly influences how your future technologies will work, so trust someone like Patoliya Infotech, which delivers high-quality software solutions and constant support.