AI in Medical Imaging Is Redefining Diagnostics and Accuracy

Table of Contents
AI in medical imaging increases the diagnostic capability and accuracy. Medical imaging generates vast amounts of structured visual data, including X-rays, CT scans, MRIs, and pathology. These situations require speed, consistency, and precision.
People naturally feel pressure when their workload increases. They rush through tasks, making accuracy difficult. This is where technology becomes critical. AI automates processes and scans images with the same level of accuracy, prioritizing critical situations for clinicians. With AI in medical imaging, the diagnosis workflow increases while accuracy remains consistent.
What is AI in Medical Imaging and Why is it Important
X-ray, CT, MRI, ultrasound, and pathological imaging help in diagnosis and treatment planning while also allowing specialists to see within the body without intrusive treatments.
Medical imaging facilitates early detection and monitoring of diseases through offering detailed anatomical and functional insights.
Advanced imaging modalities generate thousands of images per study, which increases the cognitive load on radiologists. It increases the risk of delays and missing findings.
AI in medical imaging is the use of machine learning models and algorithms to evaluate imaging data, detect abnormalities, and assist with diagnosis.
It automates analysis and prioritizes cases that are urgent, reducing burden and improving consistency in the diagnosis procedure.
How AI in Medical Imaging solves Radiology's Workload and Accuracy Challenges
AI in medical imaging reduces reporting delays, prioritizes important cases, and automates repetitive operations. This lessens the workload and accuracy issues in radiology.
Workforce Shortages and Burnout
Radiologists are experiencing chronic burnout because of growing workloads and personnel shortages. Every day challenges include lengthy reading sessions, frequent disruptions, and increasing case volumes.
This affects long-term workforce sustainability and diagnostic accuracy.
Reporting Delays in Care and Backlogs
Reporting backlogs are increasing as a result of antiquated prioritization algorithms and manual operations. Treatment timeframes can be prolonged, and diagnoses slowed down by delayed image interpretation.
This raises clinical risk, particularly in emergency imaging, cancer, and critical care.
Growing Complexity of Diagnosis
For each investigation, advanced modalities like CT, MRI, and hybrid imaging produce massive data sets. Even for experts, interpreting high-resolution and multi-sequence photos while matching clinical data increases cognitive burden.
This supports workforce sustainability by enabling radiologists to concentrate on complex interpretation and enhancing diagnostic quality.
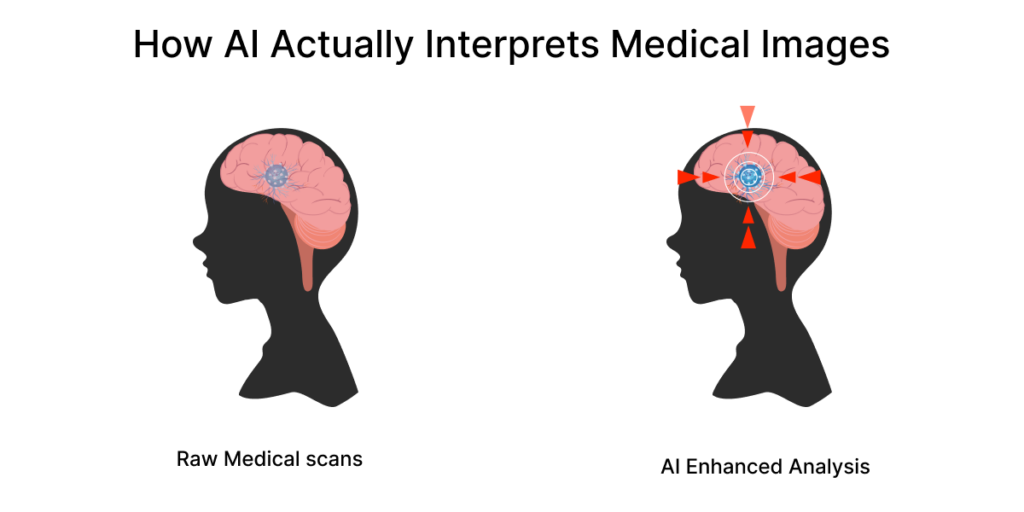
How AI in Medical Imaging Interprets Clinical Images
Deep Learning Systems to Rule-Based CAD
- Unlike radiologists, AI cannot interpret MRIs and X-rays. To find signals associated with illness, it examines patterns pixel by pixel.
- Early computer-aided detection (CAD) techniques were based on predetermined criteria such as predefined thresholds, forms, and intensity patterns. This is useful for some tasks, but systems have trouble with anatomic variation, image quality, and disease presentation.
- Advanced medical imaging using deep learning AI uses data to directly learn patterns. This model is very effective across a wide range of patient demographics and imaging settings since it fails to stick to the same principles as CAD and adapts to real-world complexity.
The Function of Transformers, CNNs, and Multimodal Models
- Convolutional Neural Networks (CNNs) are used to recognize spatial patterns in tissue anomalies, lesions, and fractures. Transformers and other modern structures enhance global context comprehension. This helps models in evaluating relationships throughout an entire research project or image.
- Multimodal AI systems that integrate imaging data with metadata, previous reports, and clinical context. In order to increase diagnostic relevance, radiologists integrate graphics with patient history, which is similar to how they think.
The Reasons for Increasing AI Accuracy and Its Limits
- Through exposure to fresh data, feedback loops, and model improvement, AI accuracy gradually increases. Prioritization at scale, consistency, and pattern detection are among its strong points.
- Even so, AI in medical imaging has limitations. It cannot reason beyond its training data, comprehend clinical complexity, and identify contexts that radiologists can detect. For this reason, AI works best as a tool for decision-making instead of as a diagnostician.
How AI in Medical Imaging Improves Workflow Efficiency
Worklist Prioritization and Intelligent Triage
AI uses real-time imaging study analysis to identify urgent instances and rearrange worklists. This guarantees that important discoveries are examined first, enhancing clinical results and turnaround times.
When internal bleeding is detected, an emergency CT scan is automatically identified and placed at the top of the radiologist's worklist.
By reorganising routine follow-up studies, significant reporting delays are minimised without human intervention.
A continuous and AI-driven secondary reader for incidental findings
AI is scanning every study for incidental or overlooked findings. This ongoing assistance increases consistency and lowers the possibility of overlooking anomalies, particularly when reporting in large quantities or after hours.
AI finds a tiny lung nodule that would have gone unnoticed during peak workload hours while examining a chest CT scan obtained for trauma.
In order to ensure prompt follow-up without prolonging the reporting period, the radiologist examines and validates the result.
Automated Reporting with Generative AI
By creating structured reports, identifying important findings, and eliminating redundant material, generative AI simplifies reporting. Radiologists spend less time on administrative duties while maintaining ultimate control.
AI creates a structured draft report with standardised terminology and measurements following image interpretation.
The radiologist reduces time on documentation and report by editing and signing off in minutes.
How AI in Medical Imaging Improves Diagnostic Accuracy
In medical imaging, accuracy is important as Modality, clinical use case, picture quality, and disease prevalence affect it. Fatigue, workload, and case complexity have an impact on human interpretation.
Therefore, a meaningful evaluation of AI in medical imaging must be task-specific to the modalities.
How AI in Medical Imaging Performs Across Imaging Modalities:
X-Ray Imaging
Where AI Is Most Effective
Because of its large volume and somewhat consistent patterns, X-ray imaging is best developed and extensively used applications of AI in medical imaging. AI models are identifying skeletal fractures and respiratory diseases like pneumonia and tuberculosis, because visual indicators stay the same across populations.
Useful Applications in Workflow
AI automatically evaluates incoming X-rays in busy emergency rooms or screening programs, identifying aberrant findings in seconds. This allows for quick priority, with normal studies being accelerated and urgent situations moving to the top of the worklist.
Clinical Role
- serves as a first-pass assessment tool in situations with a lot of traffic.
- reduces perceptual errors during periods of high workload by acting as a second reader.
- increases turnaround time without sacrificing the accuracy of the diagnosis.
CT Imaging
Why AI Is Helpful
Deep contextual knowledge is necessary for MRI interpretation, especially in neurology and cancer. Neurodegenerative indicators, tumor classification, and disease progression rely on complex, multi-sequence associations that need professional judgment.
Useful Applications in Workflow
AI helps by emphasizing areas of interest, measuring disease volume, monitoring changes, and contrasting earlier research. This enhances consistency and lessens manual labor, particularly in long-term follow-ups.
Clinical Role
- Assistance with decision-making, not independent diagnosis.
- Quantitative examination of tumor burden and development.
- Boosting confidence in situations that are unclear or complex.
- Speeds up processing without sacrificing accuracy for diagnosis.
MRI Imaging
Why AI Is Helpful
Deep contextual knowledge is essential for accurate MRI interpretation, particularly in neurology and oncology. Neurodegenerative indicators, tumor characteristics, and disease progression rely on complex, diverse correlations that call for professional judgment.
Useful Applications in Workflow
AI emphasizes areas of interest, measuring lesion volume, monitoring changes over time, and contrasting earlier research. This enhances consistency and lessens manual labor, particularly in long-term follow-ups.
Clinical Role
- Support for decisions instead of diagnosis.
- Tumor burden and progression quantitative analysis.
- Increasing confidence in situations that are unclear and complicated.
Digital Pathology
Where AI Provides Major Consistency
In digital pathology, tissue samples are analyzed under a microscope, and different pathologists interpret the results differently. AI is effective at cancer grading, mitotic count estimation, and cell-level pattern recognition. It is vulnerable to human subjectivity.
Useful Applications in Workflow
AI identifies areas of concern, pre-screens whole-slide images, and provides suggestions for uniform rating. Pathologists examine and confirm results. This decreases inter-observer variability and review time.
Clinical Role
- Confidence booster for classification and grading.
- consistency between labs and organizations.
- Enhanced reliability in the detection of cancer.
The Practical Role of AI in Medical Imaging Diagnostics
Error Reduction Without Clinician Slowness
- AI reviews every study for subtle or easily missed findings. This is useful for complex cases when human fatigue raises the risk, such as night shifts and high-volume reporting.
- AI helps lower perceptual errors and inter-reader variability, but radiologists make the final decisions. This increases uniformity without lengthening the evaluation period.
Timely Care, Prioritization, and Speed
- In actual time, AI assesses incoming imaging tests and highlights those with potentially dangerous results. The worklist is automatically updated to prioritize urgent situations. In situations where minutes count, this guarantees quicker attention.
- Improved clinical response times, better task distribution, and quicker turnaround for severe and emergencies without putting strain on staff.
Standardization Among Readers and Websites
- AI offers standardized evaluation criteria, structured outputs, and quantitative measurements. This promotes consistent reporting across departments and lessens subjective variation among clinicians.
- This increased clinical trust, repeatable reports, and increased diagnostic confidence. This is true for multidisciplinary decision-making and follow-up care.
How AI in Medical Imaging Is Delivering Measurable Impact
Stroke detection and reduced time-to-treatment
Time has a direct impact on the neurological prognosis of acute stroke therapy. As soon as CT and CTA scans are acquired, AI systems analyze them and identify any possible bleeding or major artery obstruction before manual evaluation can start.
This leads to shorter waiting times, earlier neurologist notice, and quicker worklist prioritizing. This is improving patient outcomes without adding to the workload of radiologists.
Cancer screening and early detection
AI is employed in screening programs for colorectal, lung, and breast cancer, where a lot of regular studies need to be examined consistently. AI helps radiologists by spotting minor early-stage anomalies that could go unnoticed and be missed.
This enhances early intervention, consistent follow-up suggestions, and screening efficiency.
Emergency imaging prioritization
Under extreme time constraints, imaging is constantly needed in emergency rooms. AI proactively escalates situations of trauma, bleeding, and embolism within the radiology workflow through prioritizing incoming scans.
shorter reporting backlogs, quicker emergency response times, and effective use of radiologists' time during busy times and overnight shifts.
Reduction in missed findings during routine scans
The majority of radiology's volume is routine imaging, which makes it susceptible to misses caused by weariness. AI continuously searches every study for secondary and incidental discoveries.
Rise in clinician confidence, better reporting consistency, and fewer missed anomalies. This is true in settings with high turnover.
The Role of AI in Medical Imaging for Clinical Decision-Making
| Strategic Dimension | The Reality of Common Imaging | How AI in Medical Imaging Works in Practice | Real Clinical Scenarios | System-Level Impact |
| Why Images Are Not Enough on Their Own | After acquisition, static photos and narrative reports are examined. These are unrelated to decisions made downstream. | AI converts photos into continuously useful data points that change based on the patient's state and stage of care. | Instead of being reviewed once, imaging findings are reused during interdisciplinary reviews, treatment planning, and follow-ups. | Imaging becomes an active clinical input throughout the care lifecycle and replaces passive documentation. |
| Integrating Imaging with Lab and Clinical Data | Clinicians should manually correlate imaging, EHR data, and lab results because they exist in silos. | AI creates contextual awareness through correlating imaging results with test results, vital signs, prescription drugs, and medical history. | To determine urgency, a lung CT result is read in conjunction with inflammatory markers and medical history. | Reduced cognitive strain on doctors, precise risk assessment, and fewer missed correlations. |
| Forecasting Disease Progression and Risk Stratification | Disease severity is determined following clinical decline. | AI finds early imaging patterns associated with complications, severity, or progression. | To modify the frequency of surveillance, oncology patients are categorized based on the probability of rapid tumor progression. | Proactive treatment, early intervention, and efficient utilization of clinical resources. |
| AI Imaging and Medical Health | Guidelines and demographic averages play a crucial part in treatment regimens. | AI extracts patient-specific quantitative imaging biomarkers. | Metrics related to tumor texture, volume, and perfusion influence the choice of individualized treatment. | Reduced errors in judgment, increased response rates, and focused therapies. |
| From Decision Intelligence to Reports | Imaging reports are kept for documentation purposes. | AI directly integrates insights into decision-making and care-coordinating processes. | AI-generated reports that highlight hazards and response patterns are sent to tumor boards. | Multidisciplinary judgments with a common data context that are quicker and more assured. |
Explainability, Bias, and the Reality of Trust of AI in Medical Imaging
How to Gain Clinical Trust in AI for Medical Imaging
Trust determines the Adoption of AI in diagnostic workflows. Instead of focusing on AI's strength, clinicians are concerned with its comprehensibility, equity, and reliability in healthcare.
Explainable AI: Bringing AI Decisions to Light
Clinicians can understand why an AI model reported a finding by using explainable AI (XAI) tools like heatmaps, saliency maps, and attention overlays. Artificial intelligence (AI) technologies closely match radiologists' interpretative process through visually indicating locations that impacted a prediction.
Why this matters: Transparency lowers suspicion, promotes clinical validation, and gives doctors the ability to contest or override AI outputs as necessary.
Demographic Differences and Algorithmic Bias
AI models are trained on historical data, which can involve regional biases, differences in imaging methods, and population imbalances. Performance can differ among age groups, genders, nationalities, and disease profiles when training datasets are not diverse.
Why it matters: In some populations, AI bias in imaging could end up in overconfidence, missing discoveries, or inconsistent diagnostic performance.
Federated Learning: Mitigating Bias Without Sacrificing Privacy
AI models can learn from data from several institutions without centralizing patient data with federated learning. Models share learned parameters and are trained locally. This makes it possible to be exposed to technical and demographic variation.
Why it matters: This strategy complies with data privacy laws, enhances generalizability, and lessens single-site bias. Because of this, AI is now representative of actual clinical settings.
Why Accuracy Is Not Enough to Build Trust
Trust is not ensured by high accuracy alone. Clinicians have to be aware of AI's strengths and weaknesses as well as how to use its results when making decisions.
Building trust in AI in medical imaging involves:
- Clearly defined performance limits.
- Explainability and visible logic.
- Continuous verification and observation.
- honest disclosure of constraints.
Regulatory and Legal Reality of AI in Medical Imaging
Regulation serves as the foundation of trust as AI in medical imaging moves from pilot programs to business adoption. Clinical AI can be safely scaled, governed, and validated using frameworks.
Clinical performance, safety, data integrity, and post-market monitoring are well defined under FDA and CE approval routes. Approval enables predictable market acceptance for vendors and signifies confirmed clinical value for providers. Regulation is becoming a differentiator in the marketplace.
The majority of solutions fall under the category of Software as a Medical Device (SaMD). This provides lifecycle control, transparency, and ongoing observation. Innovation is made possible without sacrificing patient safety.
Legally speaking, there is shared accountability: clinicians have the last say in decisions, while suppliers are responsible for model performance and compliance. AI does not diagnose problems on its own, and it supports decisions.
Radiology Workflow Before and After AI Integration
| Workflow Stage | Radiology Workflow Before AI | AI‑Assisted Workflow in Medical Imaging | Practical Impact |
| Acquisition of Images | Images that were collected and stored without being prioritized. | AI analyzes images instantly upon acquisition. | Faster downstream action with no change in acquisition. |
| Setting Priorities for Cases | First-come, first-served is a common method of manually arranging worklists. | AI triage rearranges the worklist and marks important instances. | Early assessment of urgent cases resulted in fewer clinical delays. |
| Visual Interpretation | A radiologist examines the complete study on their own. | AI draws attention to areas of interest and possible abnormalities. | Fewer perceptual errors and a lower cognitive load. |
| Incidental Findings | Often found when time provides. | AI constantly looks for incidental and secondary findings. | Enhanced consistency of detection without extra effort. |
| Reporting | Manual typing and formatting. | AI-assisted and automatically produced structured reports. | Standardized output and quicker report creation. |
| Time of Turnaround per Scan | Longer and more unreliable. | Reduced and more predictable. | Faster diagnosis, particularly in emergencies. |
| Workload for Radiologists | High levels of exhaustion at peak volume. | Workload balancing through prioritizing and automation. | Enhanced the effectiveness and well-being of clinicians. |
| Effects at the System Level | Reporting backlogs and care delays. | Increased productivity and efficient utilization of resources. | Total time savings across all departments. |
Measuring Success with KPIs and ROI in AI in Medical Imaging
Diagnostic turnaround time
One of the best measures of the impact of AI is turnaround time. AI shortens the time between image collecting and final report by facilitating intelligent triage, worklist prioritizing, and AI-assisted reporting. This is beneficial in critical care and emergencies.
TAT Improvement (%) = (Baseline TAT − AI-Assisted TAT) / Baseline TAT × 100
Miss-rate reduction
AI as an ongoing second reader, minimizing perceptual errors caused by exhaustion, heavy reading, or intricate research. In both routine and urgent scans, this reduces the percentage of missing and delayed results.
Miss-Rate Reduction (%) = (Baseline Miss Rate − AI-Assisted Miss Rate) / Baseline Miss Rate × 100
Cost per scan
Automation with AI lowers manual labor, rework, overtime, and reliance on outside reporting services. This preserves and enhances diagnostic quality while reducing the operating cost per scan.
Cost Savings per Scan = AI-Assisted Cost per Scan − Baseline Cost per Scan
Annual Savings:
Total Savings = Annual Scan Volume × Cost Savings per Scan
Radiologist Productivity
AI frees radiologists to concentrate on complex interpretation by lowering administrative and cognitive strain. Consistent reading volumes and decreased burnout are indicators of productivity gains.
Productivity Gain (%) is calculated as follows: (Studies per Radiologist After AI − Before AI) × Before AI × 100
Patient outcome improvements
Duration of treatment, follow-up compliance, and disease stage at diagnosis are enhanced through earlier detection, quicker prioritization, and reliable reporting.
Improvement in Time-to-Treatment (Outcome KPI):
Reduction of Treatment Time = Baseline Time − AI-Assisted Time
AI's enterprise return on investment(ROI) in medical imaging:
ROI (%) = (Annual Financial Benefit minus Total AI Investment) times Total AI Investment × 100
Financial Advantages Consist of:
- Reduction of labor costs
- reduction in overtime
- avoided the expense of outsourcing
- Decreased imaging repetition
- Increased revenue throughput
The Role of Radiologists with AI in Medical Imaging Procedures
Detection and Interpretation
AI is very effective at finding patterns and abnormalities in vast amounts of imaging data. As a result, the radiologist's role involves deeper interpretation instead of basic detection.
This connects imaging results to clinical history, the stage of the disease, and the effect of treatment.
Radiologists concentrate on complex cases, interdisciplinary discussions, and essential clinical guidance.
AI Managing High-Volume and Routine Cases
A large amount of radiology's effort is devoted to routine investigations and examinations.
AI can save human labor without sacrificing safety through pre-screening, triaging, and drafting reports for certain cases. This results in consistent workloads and increased productivity.
Radiologists as AI Supervisors and Validators
Radiologists are the last validators in AI and automated workflows. Radiologists monitor system performance, resolving uncertainties, and evaluating AI outputs.
They are essential to governance, quality control, and ongoing model development.
This results in increased accountability and trust while maintaining clinical authority.

The Future of AI in Medical Imaging
Multidisciplinary AI For Laboratories, Genomics, and Imaging
Imaging data will be integrated with labs, pathology, genomes, and longitudinal EHRs in future systems. These combinations result in a deeper understanding of diseases and accurate risk assessment.
Within a larger context of clinical intelligence, imaging becomes a predictive indicator.
Real-Time and Predictive AI Medical Imaging
AI will predict the progress of an issue, how well a treatment will work, and the likelihood of deterioration. Imaging will reveal not just what has already happened but also what is expected to happen. This helps in proactive care paths and earlier interventions.
Workflows that are autonomous and self-optimizing
Workflows in radiology will become more flexible. This involves continuously optimizing efficiency, learning from results, and self-prioritizing cases. This enhances scalable efficiency and quality under human supervision without compromising clinical control.
Conclusion
AI in medical imaging increases clinical capacity, improves accuracy under pressure, and allows radiology teams to operate at scale. As imaging volumes increase, so does diagnostic complexity. AI assists in decision-making by interpreting images in a high volume and consistent context.
Explainability, bias reduction, regulatory compliance, and human oversight are essential for responsible adoption. When AI is applied with strong governance and smoothly integrated into healthcare workflows, it leads to measurable benefits in turnaround time, cost efficiency, workforce sustainability, and patient outcomes.
Adoption of AI improves operational efficiency by making the best use of resources. It enhances financial efficiency, scalable diagnostics, consistent performance, and long-term clinical resilience.
The software vendor is responsible for the successful implementation of AI in medical imaging. A proficient professional with expertise in this field can bring long-term growth through technology. Trust someone like Patoliya Infotech, who has extensive experience in the healthcare industry and creates high-quality solutions.